Anaerobic Bacterial Infections: Overview and Clinical Implications
Anaerobic bacterial infections are caused by bacteria that do not require oxygen for growth, posing challenges in diagnosis and treatment. This article delves into the types of anaerobic bacteria, their role in human infections, and common clinical presentations such as abscess formation. Gram-negative anaerobes like Bacteroides spp. and Prevotella P. are frequently implicated in intra-abdominal and pelvic infections. Understanding these pathogens is crucial for effective management of anaerobic bacterial infections.
Download Presentation

Please find below an Image/Link to download the presentation.
The content on the website is provided AS IS for your information and personal use only. It may not be sold, licensed, or shared on other websites without obtaining consent from the author. Download presentation by click this link. If you encounter any issues during the download, it is possible that the publisher has removed the file from their server.
E N D
Presentation Transcript
University of Mustanisiriya College of Medicine Third stage Anaerobic Bacterial Infection Asst.Prof.Dr. Nadia Hameed Mohammed MBChB FIBMS Patholoy/mico-immunopath
Overview Anaerobic bacteria: Bacteria that do not use oxygen for growth and metabolism but obtain their energy from fermentation reactions. These bacteria could be Obligate anaerobes or Moderately obligate anaerobes Obligate anaerobes usually lack super oxide dismutase (SOD) and catalase and are susceptible to the lethal effects of oxygen Moderately obligate anaerobes have small amounts of both catalase and SOD and most anaerobic infections of humans are caused by this type. Facultative anaerobes: Bacteria that can grow either oxidatively, using oxygen as a terminal electron acceptor, or anaerobically, using fermentation reactions to obtain energy. Facultative anaerobes are common pathogens. Streptococcus species and the Enterobacteriaceae (eg, Escherichia coli ) are among the many facultative anaerobes that cause disease.
Anaerobic Bacterial Infection Anaerobic Bacterial Infection Caused by anaerobic bacteria wic are found as part of the normal microbiota throughout the human body and in high concentrations in the mouth and gastrointestinal tract. Infections caused by anaerobic bacteria are common. It is usually polymicrobial (anaerobes, facultative anaerobes, and aerobes), but anaerobes & facultative anaerobes are the common. Infection results when anaerobes and other bacteria of the normal microbiota contaminate normally sterile body sites. The main clinicopathological form of anaerobic infection is abscess formation.
Dermal abscess Dental abscess Source https://conciergedentalgroup.com/ blog/understanding-dental-abscess -with-concierge-dental-group/ Source https://stock.adobe.com/search?k=abscess
Anaerobic bacteria found in human infection I / Gram negative anaerobes: A. Gram Negative Bacilli 1. Bacteroides spp Very important anaerobes that cause human infection. They are a large group of bile-resistant, non spore-forming, slender gram negative rods that inhabitant bowel and other sites. Bacteroides species are most often implicated in intra-abdominal infections and pelvic inflammatory disease &tubo-ovarian abscess. B fragilis is the commonest cause of human anaerobic infection.
Gram Negative Anaerobes 2. Prevotella P. Melaninogenica associted with pulmonary abscess & empyaema. P. Bivia. Associated wit pelvic inflammatory disease PID &tubo- ovarian abscess 3. Porphyromonas They are normal oral microbiota & may occur at other anatomical sites Porphyromonas species can be cultured from gingival and periapical tooth infections
Gram Negative Anaerobes 4. Fusobacteria most human infections are caused by Fusobacterium necrophorum and Fusobacterium nucleatum F. necrophorum is quite virulent, causing severe infections of the head and neck that can progress to a complicated infection called Lemierre s disease (uncommon complicated bacterial pharyngitis/tonsillitis and involves an extension of the infection into the lateral pharyngeal spaces of the neck with subsequent septic thrombophlebitis of the internal jugular vein). F. nucleatum is a significant component of the gingival microbiota as well as the genital, gastrointestinal, and upper respiratory tracts. As such, it is encountered in a variety of clinical infections such as pleuropulmonary infections, obstetric infections, significantly chorioamnionitis, and complicating periodontal disease.
Gram Negative Anaerobes 5. Bacteria that cause bacterial vaginosis: Bacterial vaginosis is a common vaginal condition of women of reproductive age. So named because inflammatory cells are not present. Two gram ve anaerobic bacilli, Gardnerella vaginalis and Mobiluncus species, have been most specifically associated with the disease process. Vaginosis diagnosed by : fishy odor vaginal discharge, presence of clue cells, (vaginal epithelial cells covered with many gram-ve bacilli ) in wet smear, absence of inflammatory cells & absence of other common causes of vaginitis such as trichomonads or yeasts. In pregnant women, it is associated with premature rupture of membranes and preterm labor .
Clue cells/ Bacterial Vaginosis (Gram stain of wet vaginal swab) Source https://www.researchgate.net/figure/Wet-mount- appearance-of-clue-cells_fig1_340179493
Gram Negative Anaerobes B. Gram negative cocci Veillonella species are a group of small, anaerobic, gram negative cocci that are part of the normal flora of the mouth, the nasopharynx, and probably the intestine. Occasionally isolated in polymicrobial anaerobic infections,
Gram Positive Anaerobes II/ Gram positive anaerobes A. Gram-Positive Bacilli 1. Actinomyces: G+ve, non motile, non spore forming, obligate anaerobic filamentous bacteria. They are normal flora of mouth and intestine. Actinomyces israelii cause actinomycosis in human Actinomyces bovis cause disease in cattle (lumpy jaw) Actinomyces https://phil.cdc.gov/Details.aspx?pid=22293
Gram Positive Anaerobes Actinimycosis Aactinimycosis is a chronic subcutaneous granulomatous infection in which sinuses are formed & open on the surface of skin. Discharging pus containing small yellowish granules (sulphur granules) which are compact colonies of actinomyces. The jaw and cervicofacial region are the usual site of infection often following tooth extraction, however abdominal or thoracic infection can occur. Actinomycosis Sulphur granules Source of the image : https://www.researchgate.net/figure/Swelling-of-the-cheek-in-a- patient-with-actinomycosis-Note-the-possible-beginning-of-a_fig1_236976734
Gram Positive Anaerobes 2. Clostridea spp in separated lecture 3. Lactobacillus Lactobacillus species are major members of the normal microbiota of the vagina. Inhibit yeast over growth by lactic acid production from their metabolism helps maintain the low pH of the normal adult female genital tract. 4. Propionibacterium members of the normal microbiota of the skin, oral cavity, large intestine, conjunctiva, and external ear canal. On Gram stain, they are highly pleomorphic, showing curved, clubbed, or pointed ends; long forms with beaded uneven staining; and occasionally coccoid or spherical forms. Their metabolic products include propionic acid, from which the genus name derives.
Gram Positive Anaerobes Propionibacterium acnes, often considered an opportunistic pathogen, causes the disease acne vulgaris. It causes acne by producing lipases that split free fatty acids off from skin lipids. These fatty acids can produce tissue inflammation that contributes to acne formation. In addition, P acnes is frequently a cause of postsurgical wound infections, particularly those that involve insertion of devices.
Propionibacterium acnes https://link.springer.com/chapter/10.1007/978-3-319-67651-7_8
Gram Positive Anaerobes 5. Eubacterium, Eggerthella, Bifidobacterium, and Arachnia Anaerobic, pleomorphic, gram-positive rods. Found in mixed infections associated with oropharyngeal or bowel flora. B. Gram-Positive Cocci normal microbiota of the skin, oral cavity, upper respiratory tract, gastrointestinal tract, and female genitourinary system. Peptostreptococcs is the important group. These organisms have been associated with serious infections such as brain abscesses, pleuropulmonary infections, necrotizing fasciitis, and other deep skin and soft tissue infections, intra-abdominal infections, and infections of the female genital tract.
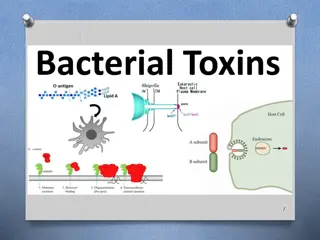
PATHOGENESIS OF ANAEROBIC INFECTIONS Infections most often are mixed infection Anaerobic infection is usually mixed with facultative anaerobic bacteria (e.g. E. Coli) as the later consuming the oxygen and thereby produce an environment in which Bacteroides species and other anaerobes can grow. Many anaerobic bacteria produce heparinase, collagenase, and other enzymes that damage or destroy tissue. The capsular polysaccharides of Bacteroides are important virulence factors. Bacteroides species have lipopolysaccharides (endotoxins) but much less toxic than those of other gram-negative bacteria. B fragilis produces a SOD and can survive in the presence of oxygen for days.
Diagnosis Clinical signs suggesting possible infection with anaerobes include the following: 1. Foul-smelling discharge (caused by short-chain fatty acid products of anaerobic metabolism) 2. Infection in proximity to a mucosal surface (anaerobes are part of the normal microbiota) 3. Gas in tissues (production of CO2 and H2) 4. Negative aerobic culture results
Treatment Treatment of mixed anaerobic infections is by surgical drainage (under most circumstances) plus antimicrobial therapy. The most active drugs for treatment of anaerobic infections are clindamycin and metronidazole. Alternative drugs include cefoxitin, cefotetan, some of the other newer cephalosporins, and piperacillin, but these drugs are not as active as clindamycin and metronidazole. Penicillin G remains the drug of choice for treatment of anaerobic infections that do not involve -lactamase producing Bacteroides and Prevotella species.
Common locations of infections involving anaerobic bacteria (Image source: Koneman, Ref-1)
1. Reidle, S., Morse, S. A., Meitzner, T., and Miller, S. 2019. Jawetz, Melnick & Adelberg s Medical Microbiology , Twenty-Eight Edition. The McGraw-Hill education, Inc. USA Centre for Disease Control and Prevention Public Health Image Library (PHIL). Levinson, W. 2016. Review of medical microbiology and immunology,14th edition. The McGraw- Hill Companies, Inc. USA Kumar, S. 2012. Textbook of microbiology. Jaypee Brother Medical Publishers (P) Ltd. New Delhi, India. 2. 3. 4. 5. https://conciergedentalgroup.com/blog/understanding-dental-abscess-with-concierge-dental- group/ 6. https://stock.adobe.com/search?k=abscess 7. 8. https://www.researchgate.net/figure/Wet-mount-appearance-of-clue-cells_fig1_340179493 https://www.researchgate.net/figure/Swelling-of-the-cheek-in-a-patient-with-actinomycosis-Note- the-possible-beginning-of-a_fig1_236976734